Written by Dr. Dana Stallings
Our most requested topic yet! Almost everyone has heard about the diabetes medications being used for weight loss. So what’s the deal??
Buckle up – this is a long one.
First things first… what are these medications? The drug class is known as GLP-1 RA – glucagon-like peptide-1 receptor agonists. GLP-1 is a receptor found on the beta cells in the pancreas (that make insulin) and on neurons in the brain. These medications stimulate the GLP-1 receptor to control the release of insulin from the pancreas; they also delay the digestion of food in the stomach, therefore reducing appetite, and aiding in weight loss.
And that’s why these medications have been flying off the shelf! In 2020, the CDC reported that approximately 41.9% of Americans over age 20 were obese. This rate has DOUBLED in the last 30 years! For many people, diet and exercise aren’t enough. However, weight loss medications have historically been largely ineffective, expensive, and difficult to obtain. And let’s face it: there are folks out there that want a “quick fix” to lose weight.
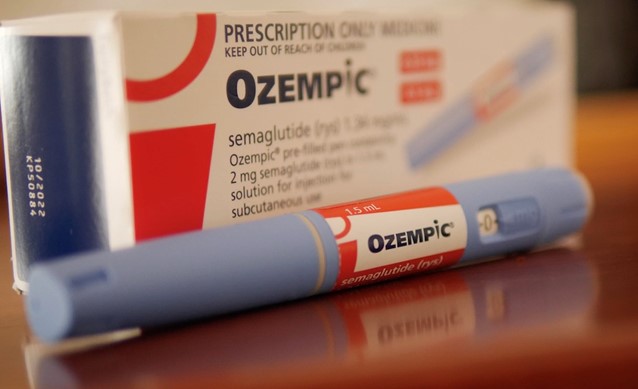
So when semaglutide (Ozempic®) hit the airwaves, people went nuts. A once weekly injectable medication that reduces appetite and helps you lose weight? Sign us up! The problem is that this entire class of medication was FDA-approved for the treatment of type 2 diabetes. When we started treating blood glucose levels with these medications, everyone noticed the accompanying “side effect” of weight loss. And because this class of medication has little to no risk of hypoglycemia (low blood sugar), people started using this medication for weight loss when they didn’t have diabetes.
And herein lies the problem. Ozempic® became so popular that the manufacturer (Novo Nordisk) could not keep up with demand. The medication went out of stock as healthcare providers prescribed it for weight loss and patients paid out of pocket for this “miracle weight loss” drug. Therefore our diabetic patients couldn’t get their prescription medication, and it all started to hit the fan. Soon thereafter, people using it for weight loss couldn’t get it either. So now, our diabetics have uncontrolled blood glucose and HgbA1c levels, and everyone else is gaining back the weight they lost!
Ozempic® is not the first drug of its kind, but they were only approved for the treatment of type 2 diabetes. It all started with exenatide (Byetta®, Bydureon®), then liraglutide (Victoza®). Liraglutide really started the weight loss craze when Novo Nordisk (yep, the Ozempic® people) rebranded Victoza® as Saxenda® for weight loss. Lilly released the weekly diabetes medication dulaglutide (Trulicity®), then Novo Nordisk followed with semaglutide (Ozempic®, Rybelsus®). Novo Nordisk then rebranded Ozempic® as Wegovy® for weight loss. In 2022, Lilly released tirzepatide (Mounjaro®).
Ozempic®, Wegovy®, and Trulicity® went out of stock due to high demand – both for diabetes and obesity. When Mounjaro® was released, it too went out of stock. They all crept back in stock, then demand hit another high, and as of this writing (August 2023) they’re almost all out of stock again. This has created a market for “compounded” medications from third party pharmacies to fulfill patient demand. Because compounded medications are not regulated by the FDA, there is a potential safety risk if not manufactured by a reputable pharmacy. Without FDA regulation, there is no way to know the manufacturing practices of third party pharmacies; therefore, we can’t know for sure which of these pharmacies are reputable and which are not. *mind blown*
This is a very polarizing topic. Not only are these great medications (my favorite class) for diabetes, they’re also critical to prevent the epidemic of obesity from morphing into even greater epidemics of diabetes and cardiovascular disease. I use these medications “on label” for type 2 diabetes, and I admittedly use these medications “off label” for other uses, including weight loss. I also write Wegovy® and Saxenda® for weight loss but insurance companies do not often cover them.
And herein lies the conundrum! What’s a patient or prescriber to do?! I don’t have the answer – because it’s not one-size-fits-all – but hopefully this article has given you a better understanding of what these medications are and why they’re in such high demand. As always, talk to your healthcare provider before embarking on any new medications for yourself. If you have questions, we’re here to help! Call Southside Diabetes 757-659-9903 to make your appointment!